Written by: Danielle Miller, MD (EM Resident Physician, PGY-2, NUEM); Edited by: Megan Quigley, MD (EM Resident Physician, PGY-4, NUEM); Expert Commentary by: Matthew Pirotte, MD
Introduction
There are two techniques for guide wire insertion when performing a central line placement. In one technique, an introducer needle is used to cannulate the vein and the guide wire is directly inserted into the needle and subsequently the vein. The disadvantage to this technique is that it requires the proceduralist to hold the needle steady as the guide wire is being introduced, and there is a possibility of needle migration out of the vessel during guide wire insertion. The other technique involves an angiocatheter over an introducer needle. Once the vessel is cannulated, the angiocatheter is threaded into the vein and the needle is removed. Then the guide wire is inserted. The advantage is that this may provide more stable venous access during guide wire insertion. The angiocatheter is also useful in manometry to ensure cannula is inside the vein (rather the the artery) in situations where an ultrasound cannot be utilized, such as subclavian central line placement. But is there truly an advantage to using the angiocatheter?
The Studies
In the study performed by Lee et al., a total of 272 patients undergoing surgery were randomized to either the use of an introducer needle alone versus the angiocatheter over introducer needle. In this study two experienced anesthesiologists who had performed both techniques over 50 times performed the central line insertions in right internal jugular veins under ultrasound guidance. The study concluded that the rate of successful guide wire insertion on the first attempt was higher in the thin wall introducer needle group compared with the angiocatheter group (87.3% vs. 77.3%; p = 0.037). There were no significant differences in major complications such as hemothorax, pneumothorax, or carotid cannulation. The overall success rate of central venous catheterization within 3 attempts was no different between the two techniques. The difficulty in first attempt with the angiocatheter was suggested to be due to the needle itself being in the vessel but the catheter, which sits slightly more proximal on the needle, not being in the vein.
In the study performed by Song et al, 132 pediatric patients age 1 day to 5 years undergoing surgery were randomized to either the use of an introducer needle alone versus the angiocatheter over introducer needle. In this study, both resident anesthesiologists and attending anesthesiologist who had each performed 50 central line insertions, performed the central line insertions under ultrasound guidance. The angiocatheter showed no superiority. There was no statistical difference in time to first successful cannulation, number of puncture attempts, or number of guide wire attempts in pediatric patients.
A third study, performed by Kim et al. had similar methods. Four hundred fourteen patients undergoing surgery were allocated to have central lines placed by 4 anesthesiologists using either angiocatheter or introducer needle alone. However, this study looked specifically at subclavian central venous catheters. Again, the introducer needle alone showed superiority. The incidence of complications was significantly lower in the needle group compared with the catheter group (5.8% vs. 15.5%, respectively, p = 0.00), and first-pass success rate was higher in the needle group compared with the catheter group (62.0% vs. 35.4% (p < 0.001).
Discussion
While the previous studies have concluded that the angiocatheter technique has no superiority, or is even inferior to the introducer needle alone, I still think there is a role for the angiocath. I would argue that the angiocatheter could have benefits in early learners. Unfortunately, the previous studies were with anesthesiologists who had performed 50+ lines. . The curriculum of central line teaching generally focuses on the introducer needle. Arguably the most difficult step in central line placement for beginners is keeping the introducer needle still as the guidewire is being advanced. The angiocath requires little skill to thread, and once the catheter is in, threading the guidewire is easy. Maybe equal time should be dedicated in teaching beginners the use of angiocath. Below is a list of instructions with pictures on how to use the angiocatheter in central line placement.
How to Perform the Procedure
1. Start the central line as usual. Wash your hands and place on sterile garb. Prep the patient’s skin, create your sterile field, anesthetize the patient, and prep the central line kit. Below the angiocath is circled in yellow.
2. Select the angiocatheter introducer needle, which is on the left in the picture below. On the right is the regular introducer needle.
As you can see in the picture below, this is what the actual angiocatheter looks like separated from the needle.
3. Cannulate the vessel with the angiocatheter introducer needle, which can be confirmed by a flash of venous blood, and on ultrasound. From personal experience alone, the angiocatheter introducer needle seems less radiopaque on US than the regular introducer needle.
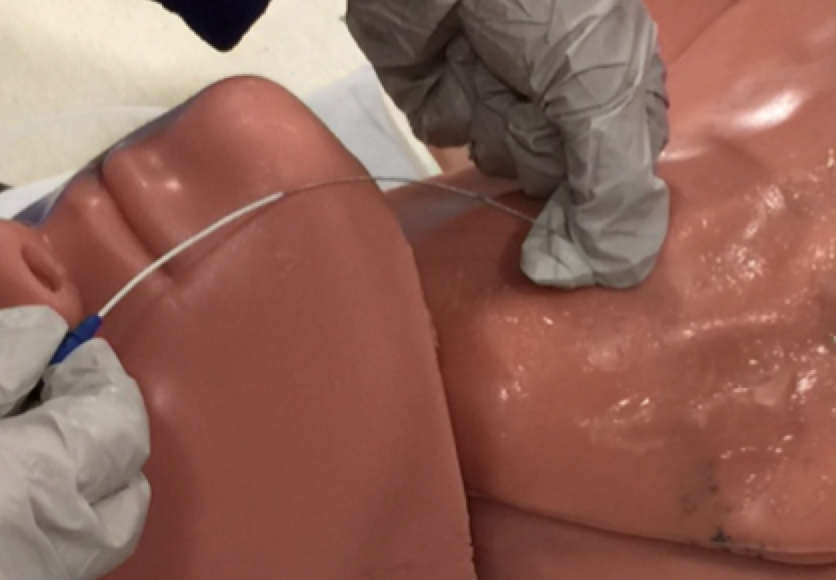
4. Holding the introducer needle steady, thread the catheter over the needle, until the catheter hub is flush with the skin
6. Remove the introducer needle and insert the guide wire into the catheter. Thread the guide wire.
7. Once the wire is threaded, remove the angiocath.
8. Continue the rest of the procedure as usual. Knick the skin with a scalpel, insert and remove the dilator, inserting the central line, flush the line, suture the line, dress the line and confirm placement
Expert Commentary
This is a nice review by Drs. Miller and Quigley of a technique I have been using for some time. Experienced operators will all agree that in patients who are significantly hypotensive, volume depleted, or experiences respiratory distress the internal jugular vein can be a dynamic and tricky target [4]. One step of IJ catheter placement that is particularly difficult is the maintaining a steady hand once the introducer needle is in the vein and ready for wire placement. We have all experienced the frustration (and more importantly discomfort to patients) of flashing nice dark venous blood only to have our guidewire fail to pass due to migration of the needle tip.
Enter the catheter-over-needle (CON) technique as an alternative and potentially superior cannulation step. While the review of these three papers is well done, the first (Lee) is really the one to focus on. The review of pediatric cases by Song et al. is certainly interesting, but most of us do not find ourselves seeking central access on young children on a regular basis. When children are critically ill in the ED the intraosseous route of IV access is an excellent and safe choice that is familiar to the majority of emergency physicians [5]. The paper by Kim et al. is similarly interesting, but I personally do not find much use for the CON technique over the standard needle approach at the subclavian site. The anatomy of a landmark guided subclavian is such that there tends to be a small amount of torque or pressure exerted on the needle because of the angle at which the operator passes under the clavicle that creates resistance to jostling of the needle during removal of the syringe and placement of the guidewire. It is also anatomically much easier for the operators to anchor the non-dominant hand against the chest and hold the needle steady after entering the vein. In all of my experience with subclavian lines, I find it very rare that the barrier to successful completion is the needle slipping out of the vein. For that matter, I am not convinced the relative thin and small bore angiocath in most central line kits would resist kinking as it passed under the clavicle in many patients.
The paper by Lee et al. represents a very nicely done study comparing the CON technique to the more standard thin-walled needle (TWN) technique. Patients were selected well and randomized; the sample had sufficient power to detect a 10% difference in rate of successful guidewire placement, which I think is a very reasonable endpoint. The authors found no difference in successful completion of the procedure although they did describe a statistically significant increase in number of punctures in the CON group. The study was not powered to detect differences in low frequency adverse events such as arterial puncture and pneumothorax.
My anecdotal experience (which should be weighed appropriately against this well done clinical trial) has been something of the opposite experience. In the interest of full disclosure, I use CON for all IJ lines and TWN for all subclavian (and femoral) lines and teach this same approach. Most residents have placed many ultrasound guided IJ lines using the TWN approach and often have never even picked up the CON apparatus. When I challenge them to try it most seem to prefer the CON approach. I have alluded to the challenges of IJ placement above, many of the lines we place in the ED are in patients who are in shock, are volume depleted, or are in respiratory distress. Holding the TWN in place while disconnecting the syringe and engaging the guidewire can often be one of the more challenging steps in placing a TLC. A careful approach with the CON method can prevent this entirely assuming the operator is successful in cannulating the vein with the full angiocath and has not malpositioned the catheter. The use of of dynamic needle tracking can facilitate successful cannulation. If placement of the angiocath is successful one need only occlude the hub with a finger to prevent air embolism while enjoying the confidence of knowing that there is no needle tip left to migrate out of or through the vein.
My final patient safety tips for those practitioners who want to experiment with the CON technique are the following:
The angiocath is somewhat fragile and attempting to reload it onto the needle after a failed attempt will often result in shearing and cutting of the catheter, because of this it is an extremely bad idea to try to rethread the needle into the catheter while the catheter is in the neck of the patient. This is unsafe and should never be attempted during troubleshooting.
The needle over which the angiocath fits is very small bore and will not accommodate a guidewire. Several times during difficult IJ placements I have seen residents use this needle “bare” so to speak when the TWN was clotted only to discover that the wire will not pass.
Matthew Pirotte, MD, FACEP
Assistant Professor; Assistant Residency Director; Department of Emergency Medicine, Northwestern University, Feinberg School of Medicine [Pubmed]
Other Posts You Might Enjoy
How To Cite This Blog Post
[Peer-Reviewed, Web Publication] Miller D, Quigley M (2017, May 16). The Use of Central Venous Angiocatheter in Central Line Insertion. [NUEM Blog. Expert Commentary By Pirotte M]. Retrieved from http://www.nuemblog.com/blog/angio-vs-needle
References
Kim et al,. A prospective randomized trial comparing insertion success rate and incidence of catheterization-related complications for subclavian venous catheterization using a thin-walled introducer needle or a catheter-over-needle technique. Anesthesia. Sept. 2016. 71(9):1030-6.
Lee, Yong Hun, et. al. Comparison of Needle Insertion and Guidewire Placement Techniques, During Internal Jugular Vein Catheterization: The Thin-Wall Introducer Needle Technique Versus the Cannula-Over-Needle Technique. Society of Critical Care Medicine. Oct 2915.
Song, In-Kyung, et al. Comparison of central venous catheterization techniques in pediatric patients: needle versus angiocath. Pediatric Anesthesia. June 2015. 25(1120-1126).
Blaivas M, Adhikari S. An unseen danger: frequency of posterior vessel wall penetration by needles during attempts to place internal jugular vein central catheters using ultrasound guidance. Crit Care Med. 2009 Aug;37(8):2345-9; quiz 2359. doi: 10.1097/CCM.0b013e3181a067d4.
deCaen A. Venous access in the critically ill child: when the peripheral intravenous fails! Pediatr Emerg Care. 2007 Jun;23(6):422-4; quiz 425-6.